With the first doses in the U.S. administered Monday, the senior living industry is close to distributing the Covid-19 vaccine among residents and staff.
In fact, senior living residents and staff could start seeing the vaccine delivered to their communities as early as about a week from now, according to Dr. Ruth Link-Gelles, who is leading the Covid-19 vaccine rollout among long-term care providers for the Centers for Disease Control & Prevention (CDC).
But before the first doses arrive, providers will need to focus on who is slated to receive the vaccine and when, how best to vaccinate new residents or employees who came to the community after the process began, and how to ensure that most people take it. Doing so is not a light undertaking, and underpinning a successful vaccine rollout are many smaller moving parts to manage.
Under the Pharmacy Partnership for Long-Term Care Program announced in October, pharmacy giants CVS Health (NYSE: CVS) and Walgreens Boots Alliance (Nasdaq: WBA) will provide and administer Covid-19 vaccines to residents and staff of long-term care facilities, including assisted living communities. While they are set to handle most of the logistics regarding distribution and administration, senior living providers are still planning ways to make the process as efficient and effective as possible.
That includes the nation’s largest senior living operator, Brookdale Senior Living (NYSE: BKD), which is preparing to “create a culture of vaccine acceptance,” according to Senior Vice President of Clinical Services Kim Elliott.
“The thing that we want to do now is educate,” Elliott said Monday during an Argentum webinar on vaccine preparedness. “It’s very important that those leaders in the communities are comfortable having the vaccine discussions.”
Collaboration is key
For providers working with CVS and its long-term care pharmacy company, Omnicare, the process will follow 10 main steps, the first of which is likely already completed for senior living operators who signed up. Before the first dose is administered, CVS plans to set up vaccine clinic dates and times for each facility or community its staff visits, distribute consent forms to each location and register patients for vaccination.
CVS asks that providers stay in frequent contact and provide current primary, secondary and tertiary contact information for their communities, according to Derek Darling, vice president of strategy, marketing and internal operations at Omnicare.
“This is certainly a massive program, but it requires all affected parties to be working in collaboration in order to be successful,” Darling said during Monday’s webinar.
Walgreens also encourages close collaboration for providers working with the national pharmacy retailer. The pharmacy will provide operators with the materials they need to prepare residents, their families and staff for vaccination, according to Tasha Polster, vice president of pharmacy quality, compliance and patient safety at Walgreens.
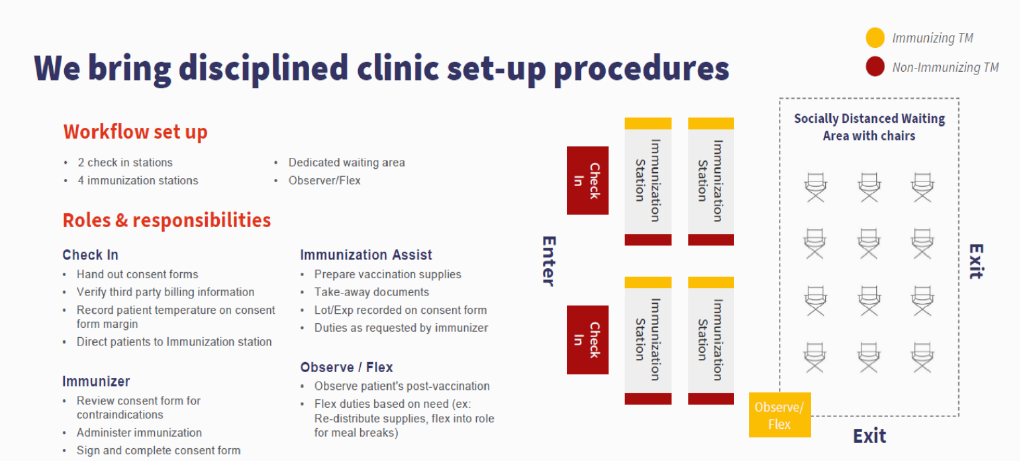
While both pharmacy providers will bring their own staff, supplies and personal protective equipment (PPE), operators should designate some space they can use for a vaccine clinic. Polster recommended a well-ventilated area with enough room to check in residents and staff, get them vaccinated and allow them to briefly rest afterward.
 Walgreens
WalgreensAs far as the logistics of vaccination itself, CVS/Omnicare and Walgreens can inoculate residents and staff in a central location, room-to-room or in a combination of the two approaches.
Although all of the Covid-19 vaccines currently hitting the market require two doses for protection against the virus, senior living operators will likely need to schedule three or more vaccine clinics to ensure everyone who wants a vaccine has gotten one, CDC’s Link-Gelles said.
“Smaller facilities may only need two clinics, larger facilities can request additional clinics,” Link-Gelles said. “We know, of course, that there are always new admissions and new staff coming on board, so that’s why the third clinic is in place.”
Getting buy-in
Although senior living operators can breathe easy knowing they aren’t in charge of shipping or storing Covid-19 vaccines, they still must compel residents and staff to take it — and that is not always easy.
Operators in the industry have tried a variety of methods to get staff more motivated to take the vaccine. Both Bloomfield, New Jersey-based Juniper Communities and Hickory, North Carolina-based ALG Senior, for example, are planning to have community leaders roll up their sleeves first to show staff and residents that it’s safe and easy to do. Others, like Birmingham, Alabama-based Atlas Senior Living, are incentivizing workers; Atlas is awarding them up to five paid days off for getting vaccinated.
Already, some large providers are optimistic that their residents are ready to get the Covid-19 vaccine. For instance, a recent survey from Sunrise Senior Living showed that 92% of the McLean, Virginia-based operator’s responding residents and their families would “definitely or probably request the vaccine for themselves, or their loved ones.”
In striving to create a culture of vaccine acceptance, Brookdale believes that education and communication are key. Elliott recommends that operators provide vaccine learning opportunities for their staff and residents — and to keep it factual.
“We’re serving that high risk population, so personal opinions or beliefs of the vaccine cannot come into play,” Elliott said. “We have to consider the CDC recommendations.”
Brookdale is also encouraging residents and their families to have discussions now with their primary care physicians to help assuage uncertainty or doubt.
And when preparing for the actual day of the clinic, Elliott recommends “digging into the details” by developing a detailed plan of attack well before the first clinic day occurs. That process should include keeping close communication with pharmacy partners, verifying and double-checking vaccine supplies against the number of residents and staff at a community, and designating roles and responsibilities for staff. Operators should also ensure the physical space is safe, efficient and clean, with vaccine clinic drills conducted in advance.
On the day of the clinic, operators should watch closely for adverse side effects in order to track and report them. Elliott also recommends that senior living companies find lessons to be learned in their first clinic in preparation of a second one.
“You have 21 days to make changes and to make the second clinic go even better,” Elliott said.
Senior living operators should also prepare to check up on residents after their first dose, even if they’ve been discharged from the community.
“If you had residents that have been discharged, what’s the follow-up?” Elliott said. “How are you going to make sure that they get fully immunized and get that second dose?”

